Surprise billing compliance: 2026 Out-of-network and Uninsured patient billing guide
January 14, 2026 | by Sarah Anderson

Out-of-Network (OON) Billing Compliance
Have you noticed how billing questions now arise even before clinical decisions are made? For medical professionals, especially those dealing with out-of-network billing and uninsured patients, cost transparency has become a frontline responsibility. Patients today expect clarity, fairness, and compliance before they consent to care. Billing compliance is no longer just an administrative duty- it is a core component of ethical, patient-centered healthcare delivery.

From a clinical operations standpoint, billing compliance ensures accurate cost disclosure, proper documentation, and adherence to surprise billing regulations. Clear good-faith estimates, advance notices, and compliant workflows protect both providers and patients. These practices reduce disputes, strengthen revenue cycle management, and align medical organizations with federal and state billing can significantly reduce administrative burden- explore Surprise Billing in Private Health Insurance: Overview of Federal Consumer Protections and Payment for Out-of-Network Services for compliance-ready billing systems.
Uninsured & Self-Pay Patient Billing Guide
When treating uninsured patients, the responsibility for transparent medical billing becomes even more critical. Explaining financial responsibility in plain, respectful language improves trust and supports informed decision-making. Consistent billing policies and compliant estimates also reduce delayed payments and write-offs. Many healthcare leaders now rely on automated compliance platforms to maintain accuracy- learn more at Surprise Billing
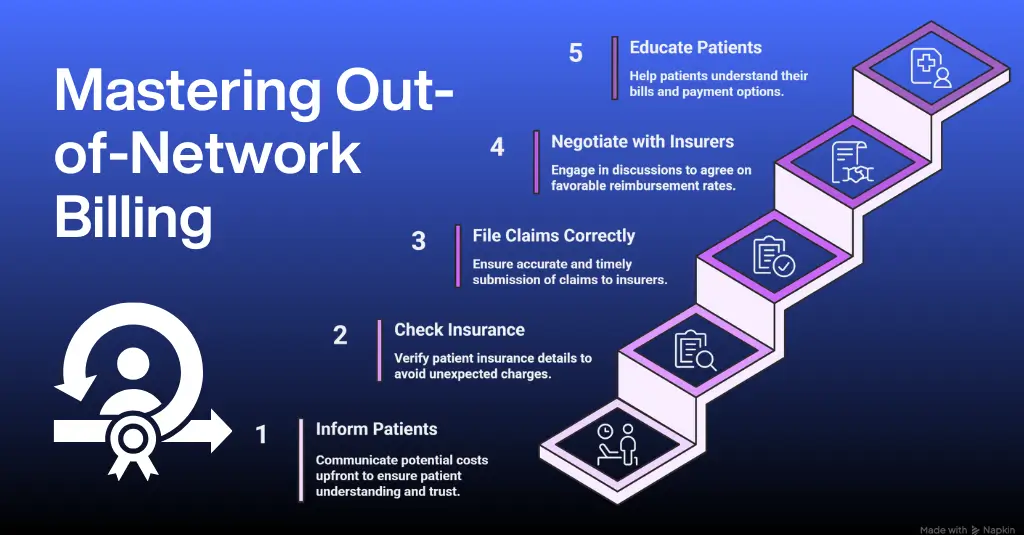
Operationally, strong billing compliance minimizes audit exposure, claim denials, and regulatory penalties. Accurate coding, staff training, and real-time compliance checks are essential for sustainable practice management. Medical organizations that invest in compliance-driven billing technology often experience improved cash flow and reduced administrative friction. A structured compliance solution can support long-term-growth see how at No Surprises Act.
2026 Operational Priorities for Providers
Ultimately, billing compliance bridges clinical care and financial integrity. When transparency replaces uncertainty, providers preserve trust while meeting regulatory expectations. Embedding compliance into everyday billing practices helps health care organizations avoid surprises, reduce mistakes, and uphold professional accountability. In a healthcare system increasingly shaped by regulation and patient awareness, compliant billing is not optional- it is a clinical and operational imperative.
Operational Infrastructure & Audit Readiness
In 2026, surprise billing compliance has shifted from a new mandate to an operational standard. Success requires a proactive approach—integrating Good Faith Estimates into every patient encounter and maintaining rigorous documentation for out-of-network services. By prioritizing transparency and automating dispute workflows, your practice can avoid federal penalties and build lasting financial trust with patients.
RELATED POSTS
View all



